What is infection?
Process by which a micro-organism establishes a colony in/on the host organism is called infection.
- If infection causes symptoms of disease in the host then – Pathogenic
- Not all infections are pathogenic
Types of Micro-organisms
- Pathogenic : those that cause infection
- Non Pathogenic : those that are not harmful
- Commensals: they live on/in the host (like symbiotic relationship) & non-pathogenic. Eg – Ecoli
- Opportunistic: they are basically commensals but become pathogenic if the hosts defense mechanism become weak.
Micro-organisms fall into 4 main groups:
- Bacteria
- Virus
- Fungi
- Protozoa
- Others – Helminths
BACTERIAL OCULAR INFECTION
What is Bacteria?
A bacterium is a single-celled (unicellular) microorganism that does not have a nucleus or any other membrane-bound organelles. Bacteria are sometimes called ‘prokaryotes.’ In Greek, ‘prokaryote’ literally means ‘before the nut’ (where ‘the nut’ is the nucleus.)
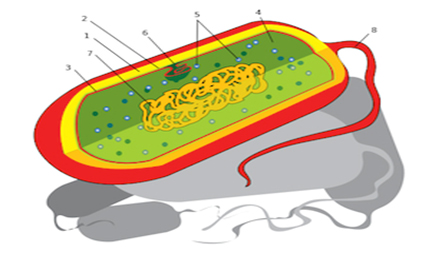
Bacteria adapt to become well-suited to their environments, and therefore come in many shapes and forms. However, they all have a few parts in common.
- Capsule: A protective, often slimy, coating, often of sugars, that helps to protect the bacterium. It also makes bacteria virulent. This means the bacteria is more likely to cause disease, since it aids the cell in survival against attack. For example, the bacteria may survive an attack from the human body’s immune system.
- Cell wall: In bacteria, the cell wall is usually made of peptidoglycan, a protein and sugar compound. This structure gives the cell some rigidity and protection.
3. Cell membrane: As in most cells, the bacterium’s plasma membrane acts by coordinating the passage of
molecules into and out of the cell.
- Cytoplasm: Again, as in many cells, the cytoplasm serves as a medium through which molecules are transported, as well as a system to maintain conditions (like temperature and pH) that are best for the cell.
- Ribosomes: The main site for the bacterium’s protein synthesis.
- Nucleosome: A basic unit of chromatin, which won’t be covered in this lesson.
- Nucleoid: This is the region where the bacterium’s DNA is located. Again, it’s not the same as a nucleus because it’s not surrounded by a membrane.
- Flagellum: In many bacteria, a flagellum is present, and is the means by which the cell moves around
Classification of Bacteria
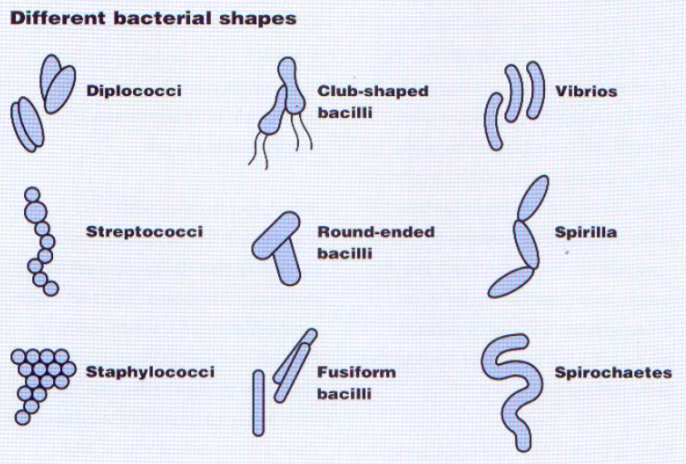
- Morphology (Cocci – round shape, Bacilli – rod shape, Vibrio – comma shape)
- Gram stain (Gram positive and Gram negative)
- Respiration (Aerobic & Anerobic)
- Colony (Clusters – Staphylo & Chain – Strepto)
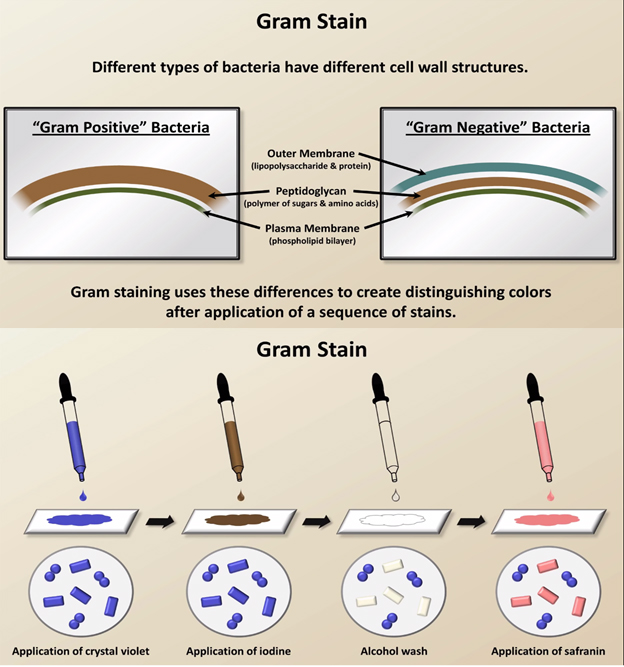
Treat first with gentian violet
Then with iodine to intensify the colour
Wash with Acetone
- Gram +ve bacteria stained violet blue
- Gram –ve bacteria decolorized
Counterstained with fuschin (stain to show up by contrast the substances already stained by another dye)
- Gram +ve bacteria remain blue
- Gram –ve bacteria stained red
Gram +ve bacterias:
- Staphylococcus aureus
Most common ocular pathogen
Transferred from skin & nail passage
- Staphylococcus epidermidis
- Streptococcus pneumonia
- Streptococcus Pyrogenes
- Corneybacterium diptheriae
Gram –ve bacterias:
- Pseudomonas aeruginosa
Multiply rapidly
Infection can become severe in ½ days
- Neisseria gonorrhoeae
Transferred to neonates during birth : Ophthalmia neonatorum
- Haemophilus influenza
- Coli
Ocular infections : Sources of Infection
- Micro-organisms around us
- Normal Flora of the eye
- Contamination
- Ocular Solutions
- Damage/trauma to ocular tissues (eg. Surgery)
- Impaired natural defense (eg. Tear deficiency)
- Predisposing conditions
Diagnosis of Ocular infection
Examination of conjunctiva
Good diffuse light
May see discharge, redness
Check lids and lashes
Examine underside of conjunctiva
Examination of Cornea
Slit lamp Biomicroscope
Stains (eg. Fluorescein) highlight damage
Corneal damage can impair vision
OCULAR INFECTIONS : TYPES OF INFECTION
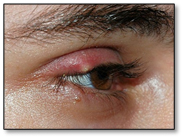
Stye : External Stye & Internal Stye (Meibomitis)
External Stye :
- inflammation of the gland at the base of the eyelashes.
- Aureus
- Analogous to a boil elsewhere
- Painful
- May burst or just subside
Internal Stye :
- Infection of a meibomian gland
- Aureus
- Rarely bursts
- If inflammation exudate accumulates it forms a meibomian cyst.
Lacrimal Apparatus
- Dacryocystitis
- Punctum becomes blocked
- Stagnating tears provide an excellent breeding ground for bacteria
Keratitis
- Inflammation of the cornea
- As an external tissue – easily infected
- Exogenous – outside infection
- Endogenous – inside infection – bacterial toxins seeping through anterior chamber
- Most common form – Corneal ulcers – sight threatening
- Redness, Grittiness, Discharge
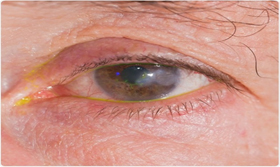
Blepharitis
- Inflammation of eyelid margins
- Often caused by Staphylococcus species
- Can be persistent and uncomfortable
- Usually not serious
- Itching, burning
- Red lid margins with crusting
- Scales
- May be associated with styes or chalazion
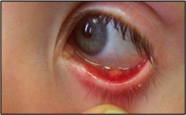
Acute Bacterial Conjunctivitis
- Inflammation of conjunctiva
- Can be acute or chronic
- Usually self-limiting
- Could be serious
Types/Causes
Bacterial
Ophthalmia neonatorum
Trachoma
Viral
Non-infectious (eg. Allergic)
Keratitis/Corneal ulcer
- Inflammation of cornea
- Very serious, sight-threatening
- Ulcer is seen as a corneal opacity
- Symptoms- Pain, Blurry vision, Discharge, Hyperemia, photophobia
Endophthalmitis
- Inflammation of internal ocular tissues
- Serious, sight-threatening
- Complication of ocular surgery
- Develops suddenly, progresses rapidly
- Symptoms – Pain, decreased visual acuity, hyperemia